There is a sound. It’s not quite a sonic boom but it’s fast and forceful. The camera cuts to birds flying out of the trees, fleeing from the danger that the sound must bring. The camera cuts to me, standing in shock. As the camera pans to a closeup of my face, you can see tears welling up in my eyes slowing, promising an overflow within moments. As dramatic music begins to swell in the background, I breathe in suddenly, as if I’d been holding my breath for hours. Suddenly, a single tear escapes my eye, my face relaxes and the audience realizes that this is a moment of relief. A release. That all is well again.
This has been one of my many fantasies that I’ve had about my cords, or axillary web syndrome, breaking or snapping. I have suffered from persistent and stubborn cording for almost three years now. And I do mean “suffered.” While I have had excellent range of motion, the cords have been extremely painful. Especially my armpit. Every time I lifted my arm, it was a tight, stretching pain. I could feel the pull go deep into my chest wall beneath my once upon a time breast and into my scar tissue, down my arm and into my hand and fingers. Does that make your skin crawl? Well, it’s not pleasant. But it was my normal. I actually got used to being in discomfort.
For those of you who don’t know what cording is, it can occur resulting from a sentinel node biopsy or axillary lymph node dissection during a mastectomy. One can develop rope or string like structures in your arm. This can inhibit range of motion and be quite painful. It is usually diagnosed by a physical therapist or lymphedema therapist (it is separate from lymphedema but can sometimes go hand it hand). It is posited that most cases for cording resolve within a few weeks to a few months with stretches and therapy. Read more about axillary web syndrome here.
But I stretched. I stretched every day. I went to therapy once or twice a week. We pulled the cord. We massaged the cord. We dug into the cord. We sang to the cord. We breathed deeply into the cord. And we definitely begged the cord. And each time, nothing. It would not move. It was intent on staying exactly where it was.
Then, last week, I was laying on my couch watching tv and I was stretching my arm and with my left hand, stretching the cord as my OT does at her office. I do this a lot in hopes that it will do something. It never does. But last week, out of nowhere I felt the most gentle pop. It wasn’t even a pop. It was an effervescence. And suddenly, in the area where I was experiencing the most pain, the pain was gone. There was some soreness where the cord had been but the rope like structure in my arm had suddenly disappeared.
Had I done it? Had I achieved the impossible? I went to be in disbelief, thinking I might have given it a good stretch. But when I woke up, it was still gone. I did it. “I got you, you fucker!!!!!!”
I had won the battle but not the war. There were still more cords. I still stretched every day. One day I felt a pop in my wrist by my thumb. I could always feel several cords there. The pop felt like when I crack my knuckles (which I sometimes do with my wrist but near my pinky, never my thumb). When I went to feel the cord, it was gone. GONE!!!!!!
Then the other day, I was stretching again, and there was a thin cord. Thin but mighty. It caused a sharp pain every time I touched it. But I was used to that pain. I pulled it. I tugged it, I dug under it and pulled it up. Nothing.
But when I woke up in the morning, it was gone. GONE!!!!! Another one bites the dust!
I always imagined that when these cords went away, that there would be tears of relief. But, the snap was so subtle and undramatic, that I didn’t know what to make of it. With the last cord, I just continued putting cream cheese on my son’s bagel as if it were a normal morning.
I know that there are still more cords that I need to snap. I can feel them and they are deep in my arm. Really deep. But I don’t feel hopeless anymore. I know that I will get them one day. My cords might be stubborn but so am I.
Did you have cording?
How long did it take for your cords to snap, if they did at all?
Do you have any magic tricks to make them disappear?
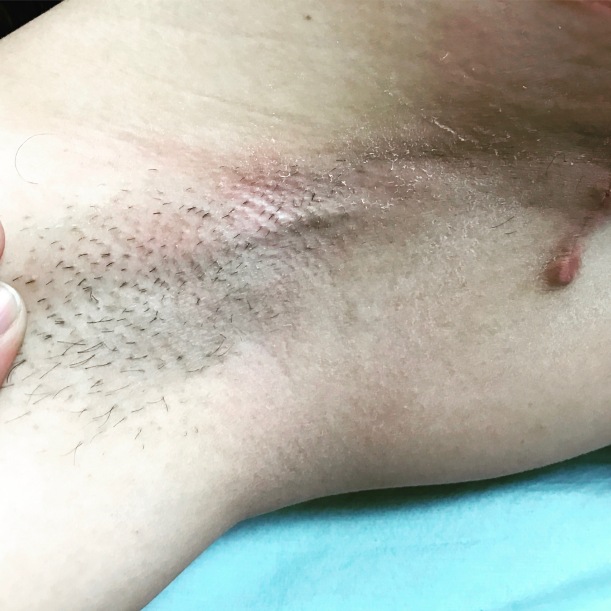
A photo taken of one of my cords. Please excuse my hairy armpits, lol! It was winter and I couldn’t be bothered.